With April comes IBS awareness month and allergy awareness week. What do both these issues have in common? You may be surprised – so read on to find out more.
First of all, do you have any of the following?
- Chronic inflammatory disease such as autism spectrum disorder, chronic fatigue and major depressive disorder
- Migraine
- An autoimmune disorder such as Coeliac, Crohn’s disease or MS
- A metabolic disorder such as obesity, gestational diabetes or Type 2 diabetes
- An intestinal disease or IBS
- A neuroinflammatory disease
- Food sensitivity
- Bloating
- Skin problems
- Fatigue
- Digestive issues such as constipation and diarrhoea
- Allergies of any type?
If you are living with one of these conditions or issues, did you know that your gut may be the cause?
Now this blog may help you start your journey to managing your most troublesome health issue once and for all.
Confused? Let’s start from the beginning.
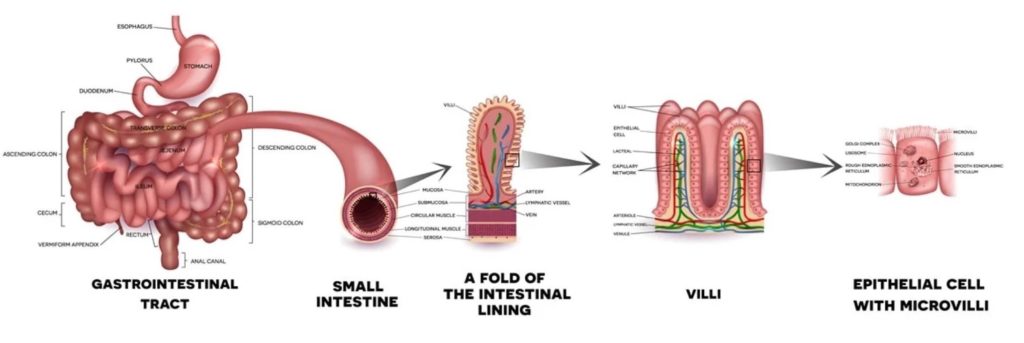
Your gut and how it works:
Inside the bowel there is a single layer of cells which make up the mucosal barrier (the barrier between the inside of the gut and the rest of the body).
This barrier can absorb nutrients, but it doesn’t let most larger molecules or germs pass through the bowel and into to the bloodstream.
Sometimes, this barrier can become less effective and “leakier”. Some things make this more likely, and we’ll cover that later.
Part of your immune system includes the gut bacteria which live in your gastrointestinal tract and ward off viral invaders. It’s thought that nearly 100 trillion bacteria, fungi, viruses and other microorganisms live inside your gut. These include bad bacteria which, in turn, are flushed out by a protein called zonulin.
It’s possible that people with more zonulin have a more permeable intestine, and then this “leaky” gut (which doctors call intestinal permeability) enables germs, bacteria and toxins to enter the bloodstream contributing to the issues in the bulleted list above. Bacterial overgrowth and gluten can also be behind overproduction of zonulin.
Over recent years the microorganisms in our gut have been linked to a range of diseases and conditions, from diabetes to autism and anxiety to obesity. They have also been associated with how we respond to certain drugs, including chemotherapy, and even how we sleep.
What’s stopping your microorganisms from doing their job?
The microorganisms in our bodies exist to support the immune system, give nutrients to our cells and stop harmful bacteria and viruses attacking us. They find it harder to do their jobs when we are:
- Taking antibiotics frequently and when it’s not 100% necessary
- Eating excessive sugar through processed food (the sugar feeds the bacteria)

- Drinking chlorinated or fluoride-added water
- Drinking too much, too often
- Eating lots of processed food
- Using antibacterial soup and products containing triclosan
- Eating non-organic meat and animal products as they are fed low-dose antibiotics and GE grains
Some things we can take or use every day are also very well known to be irritants of the bowel lining. This includes ibuprofen, aspirin, alcohol and anti-inflammatory drugs. They can allow some substances to pass through the gaps and into the blood stream as they damage the seals between cells. Sometimes, this can lead to you having ulcers in your bowel lining.
What about food intolerances and allergies?
‘Let food be thy medicine and medicine be thy food” – Hippocrates
An allergic response to food ranges from slight irritation to anaphylaxis- a life-threatening immune reaction that needs immediate medical attention.
Over the years, increasing research has shown that there are some factors which make food allergies more likely. These include c-section delivery, antibiotic use, lack of exposure to microbes in early childhood and a high fat/low carb diet.
There also appear to be huge differences in the gut microflora with people living with food allergies compared to those living without. Interaction between bacteria such as Bacteroides, Enterobacteria, Bifidobacterial and Lactobacilli within the intestinal system seems to somehow train the body to tolerate food triggers. Where the gut flora contains fewer of these key bacteria, there seems more chance of allergies developing.
On the other hand, intolerances are caused by inflammation in the gut, and once that has been resolved small amounts of the offending food can be reintroduced gradually until you build full tolerance to them again.
What about seasonal allergies?
It’s likely that our gut health also affects other allergy related health issues – in particular, asthma. One reason for this may be that we are too clean! These days, the plethora of antibacterial soaps, sanitisers and powerful germ-killing products we use in our homes are changing the microbes in our gut. This means that our immune systems are no longer frequently challenged, so we’re more likely to get allergic to our environment.
It may also be possible that as temperatures rise across the globe, the pollen allergy season is becoming longer and more intense. The Lancet Planetary Health reported that there’s an important link between global warming and public health which could be exacerbated as temperatures continue to rise.
Whether you’re living with laboured breathing, a blocked up nose, weeping eyes or any other allergy symptoms, you’d be wise to keep your gut microbes as healthy as possible.
“One month on and I’m a different person! I’ve had no hay fever symptoms so far this spring and my dust allergy is a thing of the past! I still get the odd headache, but I’ve learned how to reduce them using the breathing techniques and I’ve still had no migraines at all! The tinnitus has gone, and the digestive problems are well under control. I’m also about 7lbs lighter and much slimmer.” – Claudia
For maximum wellness and Total Health Now Clinic, we can help:
What can you be doing to support good gut health? What small changes can you make to your life to improve your general wellness? How can you manage your gut health, diet and lifestyle if you’re living with any of the issues mentioned in this article? We are here to help.
Read more about assessing the health of your digestive system here, learn more about how to cleanse and detox your gut here and book a free 20 minute telephone consultation on this link.